- Еуромедик, Булевар уметности 29, Београд
MASTITIS
Проф др Љиљана Букарица
Прим др Милош Почековац
Шта је маститис?
According to the World Health Organization, mastitis is an inflammation of the breast tissue that may or may not be related to a bacterial infection.
There are different types of mastitis:
Neonatal mastitis
Neonatal mastitis is a rare, acute bacterial infection of the breast tissue. It usually occurs on one breast, but it is possible that both breasts are affected by the infection. It occurs a few days after childbirth, usually during the first two weeks, and is manifested by swelling, redness and increased body temperature. The most common causative agent is Staphylococcus aureus, although sometimes Escherichia coli, group B Streptococcus, Peptostreptococcus, Bacteroides can also be present. In the early stages, antibiotics can control the infection, however, if there is a localized collection on ultrasound, an incision should be made. Although it is easy to perform excision of the entire lesion at this stage of development, such a procedure usually leads to secondary amastia. Also, the incision around the nipple should be avoided, if possible, and only needle aspiration should be performed and antibiotic therapy should be administered.
Cutaneous mastitis
Cellulitis is a rare breast infection that can be difficult to distinguish from inflammatory breast cancer or benign erythematous breast changes. Pain is a prominent feature of cellulitis associated with erythema, swelling, and warmth. Treatment is with antibiotics.
Epidermoid cysts are discrete nodules in the skin, which are often called sebaceous cysts or atheroma. These cysts are common in the skin of the breast and can become infected, forming local abscesses that are best treated with a small incision and drainage rather than aspiration, as the material in the abscess is too thick to aspirate.
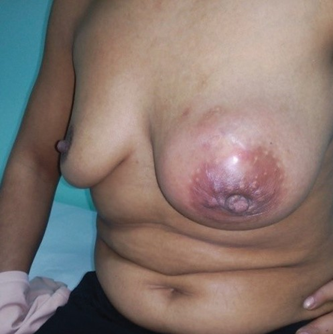
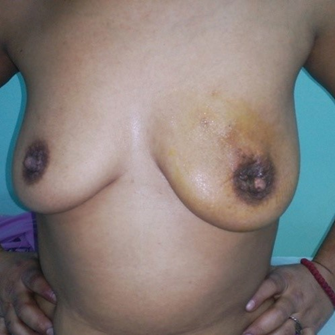
Непосредно после инцизије у амбулантним условима
Nipple piercing
Putting an earring on the nipple can lead to subareolar breast abscess and occasional nipple infections, especially in smokers. One study indicated that nipple piercing was a significant risk factor for subareolar breast abscess, especially in smokers.
Pilonidal sinuses
Pilonidal nipple sinuses have been reported in groomers and sheep keepers because the hairs penetrate the skin and can lead to inflammation and infection.
Lactation mastitis
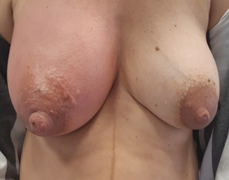 Mastitis most often occurs postpartum during the second and third weeks, and most studies have shown that between 74% and 95% of cases occur in the first 12 weeks. However, it can happen at any stage of lactation, including the second year. A breast abscess is also most common in the first 6 weeks after delivery, but can occur later.
Mastitis most often occurs postpartum during the second and third weeks, and most studies have shown that between 74% and 95% of cases occur in the first 12 weeks. However, it can happen at any stage of lactation, including the second year. A breast abscess is also most common in the first 6 weeks after delivery, but can occur later.
Lactational mastitis occurs in 2.5% of nursing mothers.
There are two main causes of mastitis: milk flow and infection.
Lactation occurs when milk cannot be adequately drained from the breast. This can happen when the milk production is accelerated after breastfeeding or at any time when the infant is not taking the milk that has already been produced.
The causes that lead to stasis are ineffective breastfeeding, poor attachment of the infant to the breast, uneven frequency and time of breastfeeding and blockage of the milk ducts. Mechanical factors such as a short frenulum in an infant (ankyloglossia), stiff and tight bras can lead to milk leakage.
In order to avoid the milk trail, it is best to start breastfeeding immediately after giving birth.
James Nelson in 1753.
If the obstruction is not removed through massage or intensive breastfeeding, there is a progression to the next stage, the so-called non-infectious inflammation characterized by pain and swelling in the area of obstruction, breast skin erythema. Milk cultures taken at this stage are sterile, but the number of leukocytes is increased (over 1,000,000/ml of milk).
Mastitis outside lactation
Mastitis that occurs outside of lactation can affect breast tissue in the central quadrant or peripherally.
Periareolar infection most often occurs in young women around the age of 32. It occurs more often in smokers. The main pathological process is periductal mastitis. The cause can be aerobic and anaerobic bacteria, autoimmune diseases. It can present as an infection around the areola with or without the presence of swelling or as an abscess collection or as a periareolar fistula. Reactive lymphadenopathy is also common. Patients without swelling should be treated with antibiotics. If there is no positive response, it is necessary to perform an ultrasound examination to determine whether there is a purulent collection. If there is an abscess, it is necessary to perform needle aspiration and antibiotic therapy or make an incision. After the inflammation subsides, a mammogram should be performed in patients over 35 years old, because very rarely a combination of infection and ductal carcinoma in situ can occur. Half of the patients with periareolar infection have repeated episodes of infection. The only effective long-term treatment for these women is surgical removal of all ducts.
Ductal canal fistula
A ductal fistula is a communication between the skin, usually in the periareolar region, and the main retroareolar duct of the breast. Fistulas most often occur after incision of an abscess, although they can occur after spontaneous discharge of a periareolar inflammatory mass or after biopsy of periductal mastitis. Patients usually complain of frequent episodes of spontaneous evacuation of the abscess collection from the ductal channel through the skin. The therapy is surgical and consists of opening the fistula or excision.
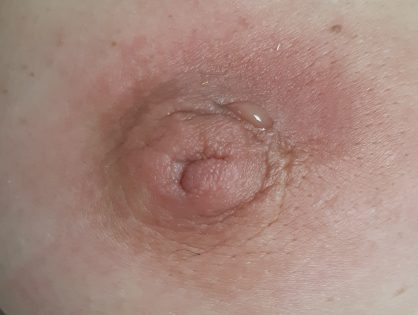
Peripheral breast abscess
Peripheral extralactational abscesses are less common than periareolar abscesses. It is usually associated with various medical conditions, such as diabetes, rheumatoid arthritis, in patients receiving corticosteroid therapy, and after trauma. Staphylococcus aureus is usually present, but some abscesses contain anaerobic organisms. Peripheral abscesses are three times more common in premenopausal women than in menopausal or postmenopausal women. Mammography is mandatory for women over 35 years of age to exclude the possibility of ductal carcinoma in situ. Abscess therapy is the same, aspiration or incision and drainage
Granulomatous lobular mastitis
A rare chronic inflammatory disease first described in 1972 by Kessler and Volok. The etiology is unknown, although it is assumed that the cause is an autoimmune process, undetected microorganisms, the use of oral contraceptives, or a reaction to childbirth. Granulomatous lobular mastitis presents as a solid tumor mass, often indistinguishable from breast cancer. Nipple retraction and sinus formation may occur. Regional lymphadenopathy may be present in up to 15% of cases. They can occur as multiple, recurrent abscesses. It is also difficult to distinguish from infectious mastitis and inflammatory breast disease.
Some patients describe a soft tissued or painful sensitive structure, and the skin above is ulcerated. It can occur in any quadrant of the breast, but is rarely bilateral. They are mostly young women, often within 5 years after giving birth. Unlike periductal mastitis, it is common in Asian rather than Caucasian women. This condition may be associated with hyperprolactinemia.
Diagnosis is made by core biopsy or surgical excision.
Some authors state that local excision with or without corticosteroid therapy gives the best results.
IF YOU NOTICE THE FIRST SIGNS OF MASTITIS, BE SURE TO CALL YOUR DOCTOR!!!
Literature
1. World Health Organisation. Infectious Mastitis. Mastitis causes and Management. Geneva: WHO; 2000.
2. William L, Weston and AT Lane. Neonatal dermatology. In: Fitzpatrick TB, Eisen AZ, Wolff K, Freedberg IM, Austen KF, editors. Dermatology in general medicine. vol 4. New York: Mc GrawHill;1993. p. 2941−60.
3. Harris JR. Lippman M.E., Morrow M. ,Osborne K.C.Diseases of the breast 5th ed. 2014.
4. Gollapalli V, Liao J, Dudakovic A, et al. Risk factors for development and recurrence of primary breast abscesses. J Am Coll Surg 2010;211:41.
5. Dixon JM. Breast infection. In: Dixon JM, ed. ABC of breast diseases. 4th ed. d. London: Wiley-Blackwell 2012.
6. Dixon JM. ABC of breast diseases: breast infection. Br J Med 1994; 309(6959): 946−9.
7. Loffler CA, Macdougall C. Update on prevalence and treatment of methicillin-resistant Staphylococcus aureus infections. Expert Rev Anti Infect Ther 2007;5(6):961-81.
8. Jonsson S, Pulkkinen MO. Mastitis today: incidence, prevention and treatment. Annales Chirurgiae Et Gynaecologiae.Supplementum, 1994, 208:84-87.
9. Kaufmann R, Foxman B. Mastitis among lactating women: Occurrence and risk factors. Social Science and Medicine, 1991, 33(6):701-705.
10. Kessler E, Wolloch Y. Granulomatous mastitis: a lesion clinically simulating carcinoma. Am J Clin Path/1972;58:642-646
11. Jorgensen MB, Nielsen DM. Diagnosis and treatment of granulomatous mastitis. Am J Med 1992;93:97-101
12. Patel RA, Strickland P, Sankara IR, Pinkston G, Many W, Rodriguez M: Idiopathic granulomatous mastitis: case reports and review of literature. J Gen Intern Med. 2009, 25 (3): 270-273.
13. Alper Akcan, A. Bahadir Öz,* Serap Dogan, Hülya Akgün, Muhammet Akyüz, Engin Ok, Mustafa Gök, and Tutkun Talih :Idiopathic Granulomatous Mastitis: Comparison of Wide Local Excision with or without Corticosteroid Therapy Breast Care (Basel). 9(2): 111–115. 2014
14. Akbulut S, Yilmaz D, Bakir S. Methotrexate in the management of idiop athic granulomatous mastitis: review of 108 published cases and reports ts of four cases. Breast J 2011;17(6):661–668.
15. Hughes LE, Mansel RE, Webster DJT. Infections of the breast. In: Hughes LE, Mansel RE, Webster DJT, eds. Benign disorders and diseases of the breast: concepts and clinical management. 3rd ed. London: WB Saunders 2009.