- Еуромедик, Булевар уметности 29, Београд
PERCUTANEOUS BIOPSIES OF BENIGN BREAST CHANGES
Доц. др сци. мед. Наташа Првуловић Буновић
мр. др сци мед. Сава Стајић
мр. др сци мед. Сава Стајић
The task of the radiologist in the breast team is to provide patients with a cytological or pathohistological diagnosis with imaging of the observed change in a fast and non-invasive way. Percutaneous needle biopsies of the breast are the standard in clinical work due to their high sensitivity and specificity. The benefit of these procedures is that they reduce the need for excisional biopsies and play a role in the decision on the method of oncological treatment. Guidelines on the role and task of radiologists in performing these procedures were given by the European Association for Breast Imaging (EUSOBI) and every radiologist in Serbia, if he has the technical capabilities, performs the procedures according to their recommendations (1).
Fine needle biopsy of the breast (aspiration biopsy) or FNAB
Aspiration biopsy is a simple and quick procedure to evacuate cyst contents (fluid contents) from the breast. The obtained liquid content can be processed in the laboratory, especially in cases of breast inflammation, when we require a bacteriological analysis (biogram and antibiogram), but the content of cystic or solid changes can also be analyzed histologically. FNAB is performed to determine the nature of the change and make an adequate treatment plan.
The procedure is performed with the patient lying on her back, side or semi-side depending on the localization of the change. The region where we will perform the puncture is wiped with a disinfectant, local anesthetics are applied and the puncture is performed, usually with a 18-23G needle. Puncture control is usually done by ultrasound. A sample of fluid or cells is smeared on a glass slide and sent to a pathologist-cytologist for analysis.
To perform the FNAB procedure, no preparation of the patient is required, no laboratory analyzes are required. Puncture can be performed easily and quickly in outpatient settings. Only disinfectant, a needle and a syringe are needed for the performance.
The purpose of the puncture is to evacuate the contents, in order to relieve the patient of the problems caused by the cysts (pain, tension, discomfort), so we consider such a puncture to be therapeutic.
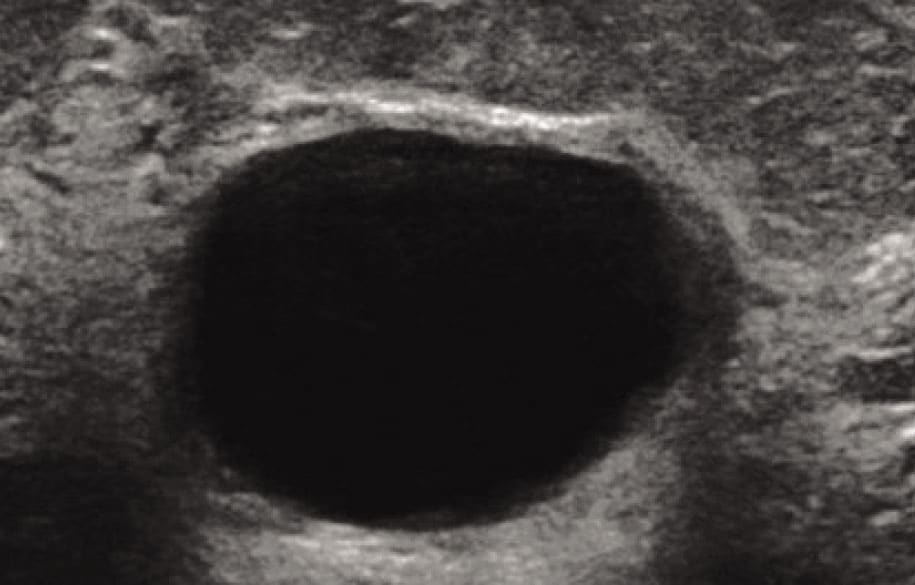
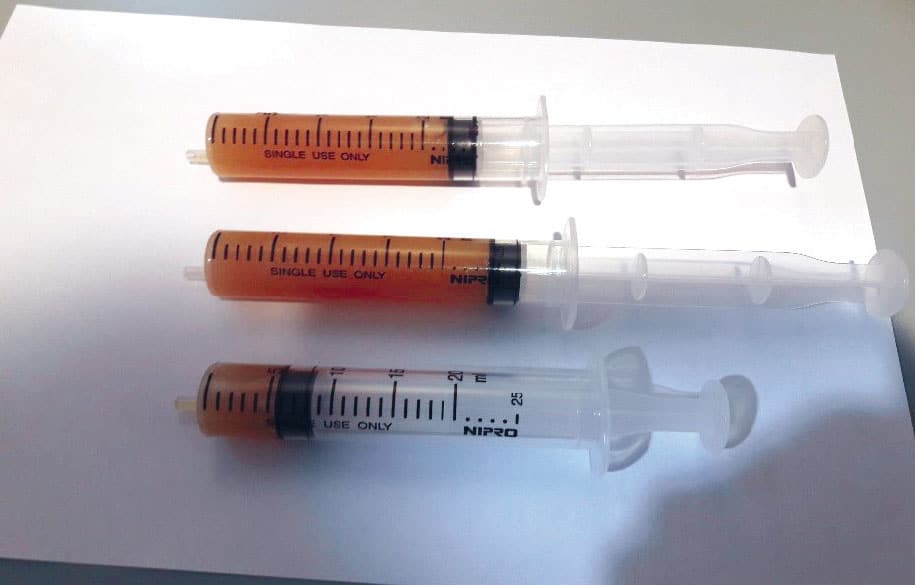
Слика 1.
Ultrasound image of a simple tension cyst in the breast and image of content after puncture (about 45 ml of clear yellowish content was evacuated).
Regardless of whether or not the patient has subjective complaints, we sometimes have the opportunity to perform a diagnostic puncture, due to the radiological presentation of a cyst or a solid change, in order to obtain an adequate cytological diagnosis.
An experienced surgeon can “simply” and easily puncture the contents of a palpable cyst or perform FNAB of solid changes, but it is more reliable to perform this procedure under ultrasound control. The procedure is more precise for changes of smaller dimensions, deeper changes, and changes that are not palpable. Rarely, the change is punctuated stereotaxically, under the control of a mammogram.
If the contents of the cyst are clear and yellowish in color, they do not require special care or treatment. If the content is mixed with pus or blood, depending on its appearance, we refer the punctate to further laboratory analysis. The contents can be analyzed bacteriologically and/or cytologically, when looking for atypical cells.
In the presence of bacterial content in the cysts, the therapy is antibiotic, per os or parenteral, depending on the degree of clinical presentation of inflammation or infection. In the case of a positive cytological finding after FNAB, a fine needle biopsy can be performed to provide material for pathohistological analysis, or the change can be surgically excised, with preoperative ultrasound marking.
The procedure carries a small risk of complications. The most common are: pain at the puncture site, minimal bleeding (especially in patients on anticoagulant therapy), bruising, while the risk of infection is very small since the procedure is performed with single-use needles with prior skin disinfection. Rare complications described in the literature are implant perforation or pleural perforation and artificial pneumothorax.
The aspiration puncture procedure is not highly sensitive and specific, if cytological analysis is performed. The obtained cytological findings must be interpreted in accordance with the clinical picture, the appearance of the punctate and the radiological presentation of the change.
Ultrasound examination of the axilla combined with FNAB can detect micrometastatic disease in 30-40% of cases, and according to research by Deurlo et al., it can reduce the need for sentinel node biopsies in about 14% of patients.
Fine needle biopsy: KOR biopsy or vacuum assisted biopsy.
Modern treatment of changes in the breast, regardless of the nature of the change, rests on its percutaneous histological verification, which, along with the localization and determination of the size of the change, will determine the method of treatment. Biopsy of changes in the breast and the resulting material, which we refer to pathohistological analysis, can be performed in two ways, using two types of devices: biopter for core biopsy (thick needle) and biopter for vacuum-assisted biopsy (VAB). A thick needle biopsy is performed with the same device used to biopsie lesions of other organs.
The advantage of biopsy over cytological analysis is that it allows preoperative establishment of an accurate histological diagnosis. Numerous studies on a large sample showed a higher sensitivity and specificity of core biopsies compared to FNAB results. The sensitivity in the detection of changes was 68-94% in cytology, 84-99% in pathohistology, and the specificity in differentiating benign changes from malignant ones was 88-100% in cytology and 99-100% in pathohistology.
Today, both types of biopsies are used equally, with a tendency to use VAB more often due to the larger amount of material obtained and thus more reliable histological diagnosis.
According to current trends, biopsy with a thick needle should be performed under the control of some imaging method, so that the process of tissue sampling is more reliable, simpler, faster and, most importantly, safe. Imaging methods should enable the control of the procedure, to “guide the needle” during the biopsy, in order to obtain the sample from the most representative place and to avoid unnecessary complications. In practice, ultrasound is most often used for core biopsies, as a modality for intervention planning and control. As a rule, all changes that are palpated or detected using ultrasound are also biopsied under the control of this method, due to simple execution, lower costs and are performed without radiation.
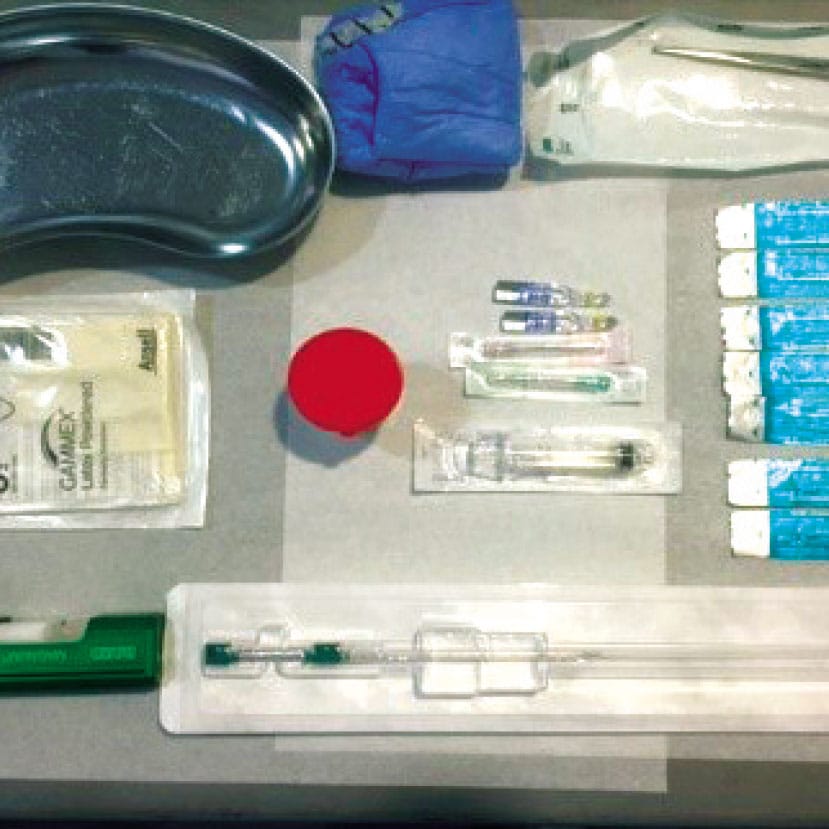
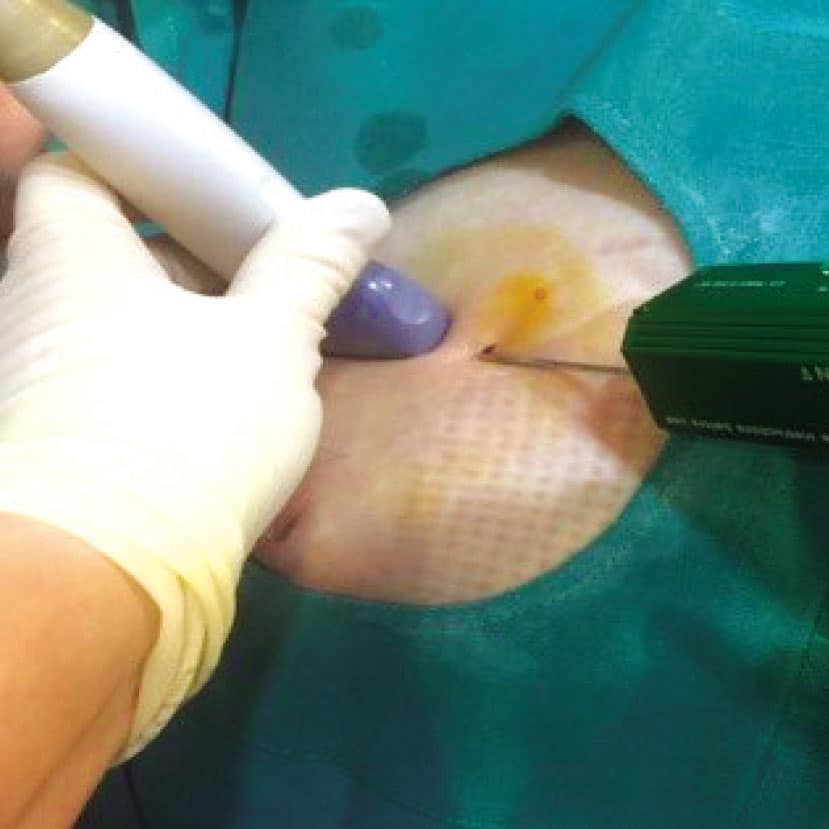
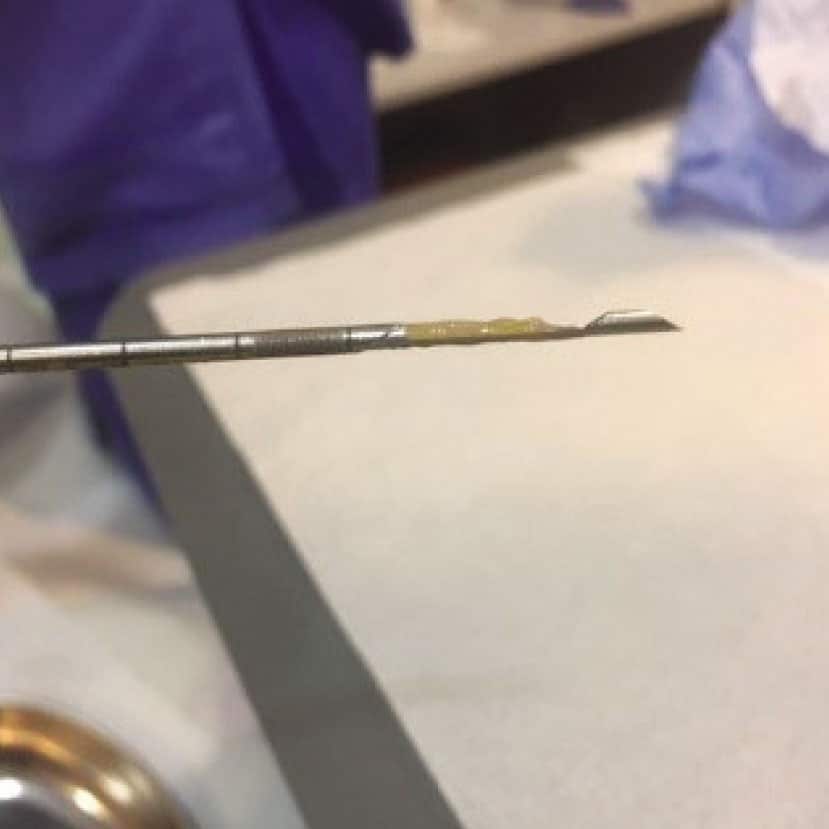

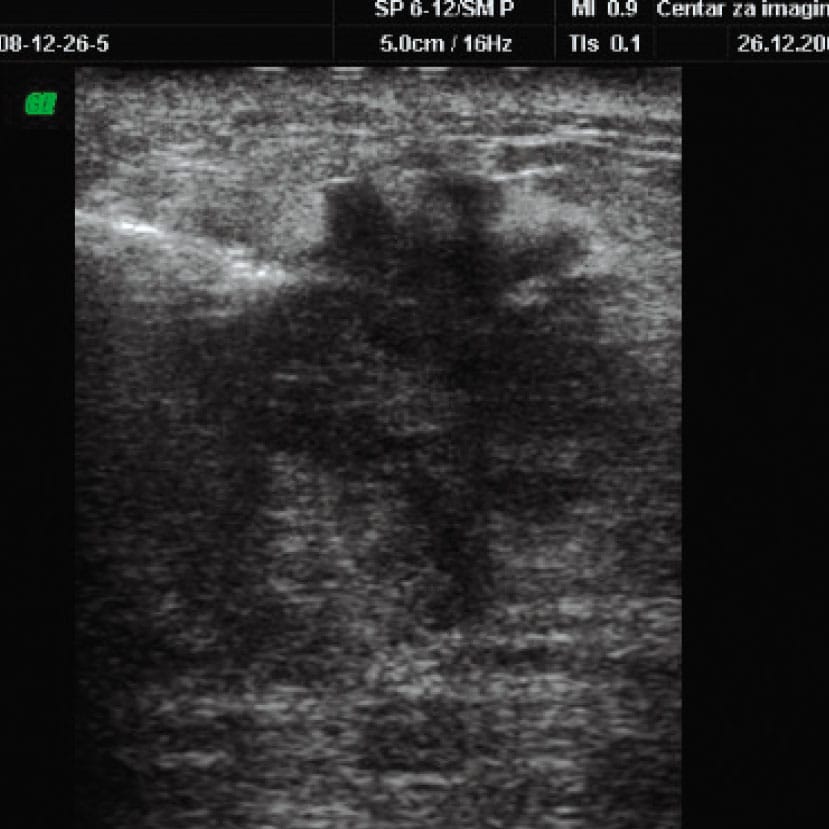
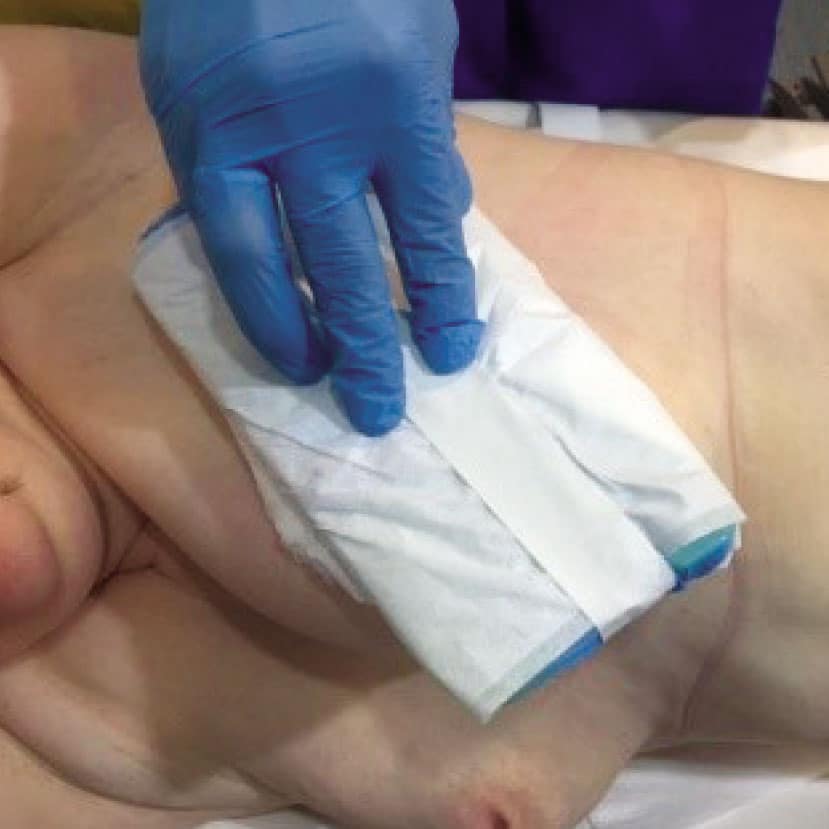
Слика 2. Припрема и извођење кор биопсије промене у дојци под контролом ултразвука.
Stereotaxic vacuum-assisted biopsy is performed under the control of a mammogram (x-ray), and a specially designed biopsy system is necessary to perform this method. This system can be incorporated into the mammograph, subsequently upgraded to the existing mammograph, or it can be a separate unit (a specially constructed system consisting of: a bed for the patient attached to the digital mammograph), with a special workstation that gives commands and controls the needle during intervention , as well as a vacuum biopter. In our conditions, in everyday practice, VAB interventions, due to their complexity, duration, use of ionizing radiation and high cost, are used in cases where changes cannot be reliably biopsied using ultrasound, which are the most common areas of microcalcifications, with or without an underlying tumor mass.
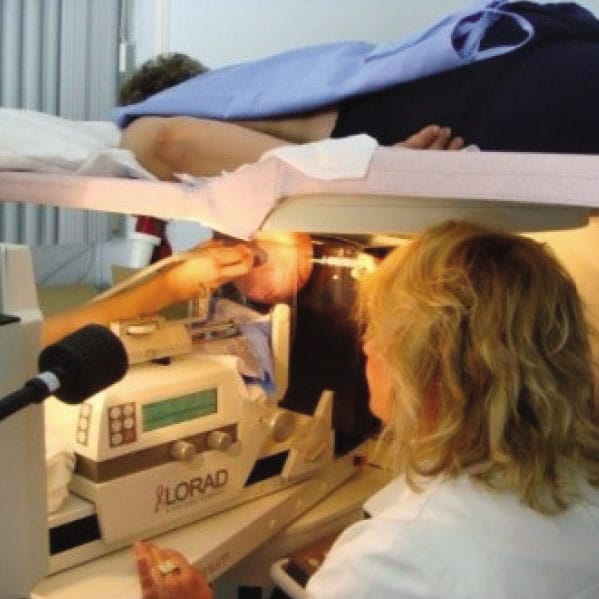
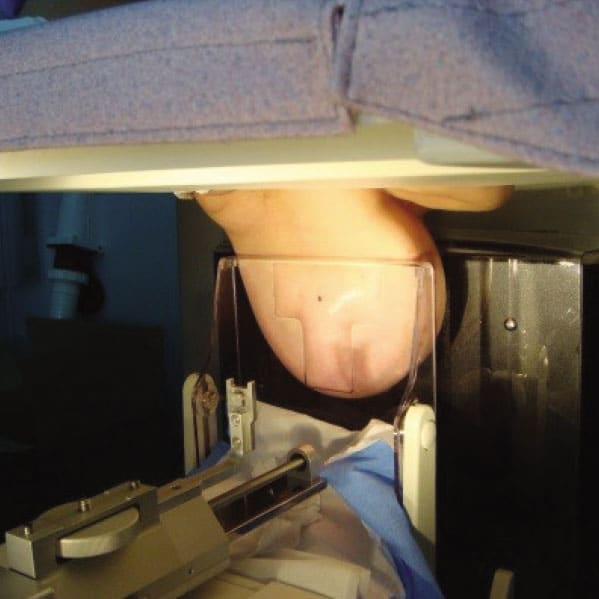
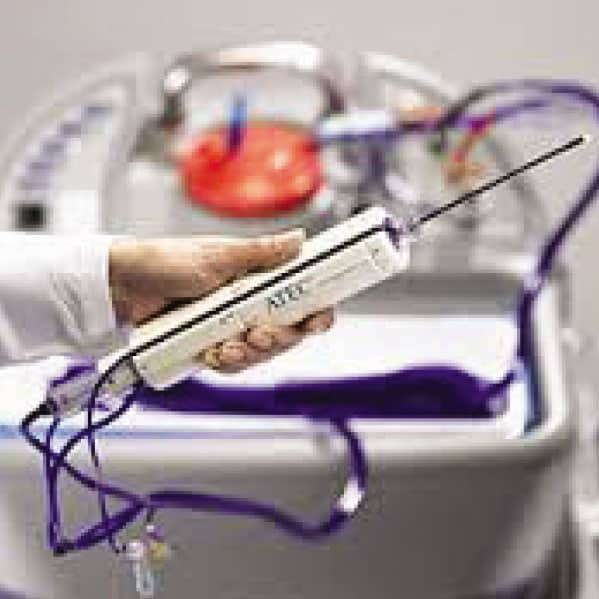
In more developed, richer countries, the use of VAB interventions is more common, over core biopsies, due to the larger volume of sampled tissue, which allows pathologists to make a more reliable histological diagnosis.
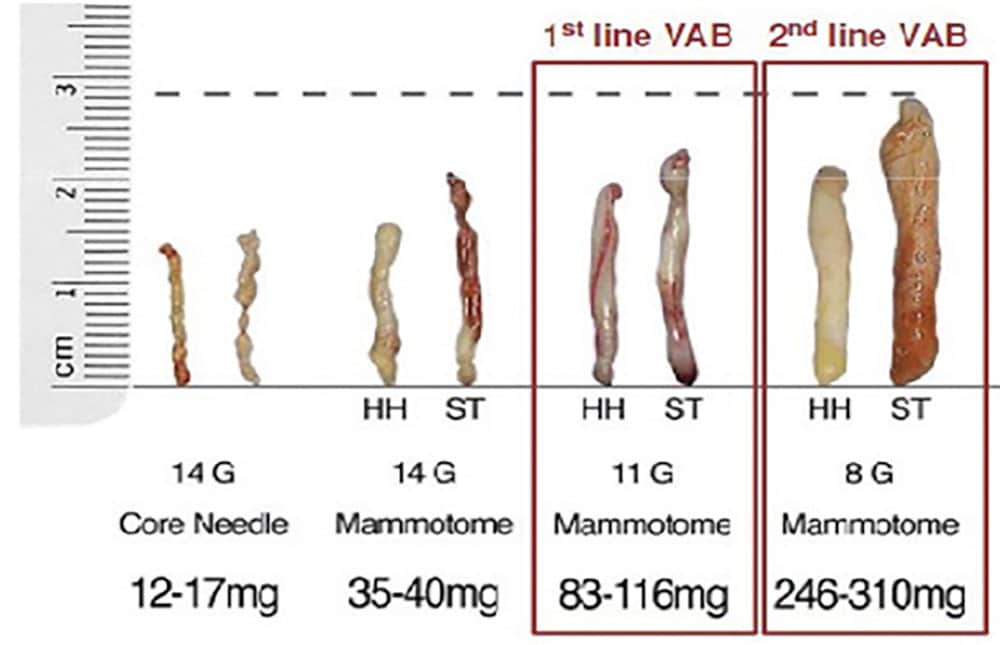
Приказ различитог волумена биоптираног ткива, зависно од врсте употребљеног биоптера и игала
(преузето са сајта: www.gov.uk/government/publications)
Each of the mentioned methods has its advantages and limitations in daily use. Depending on the knowledge and skill of the radiologist performing the procedure, the outcome of these interventions will also depend.
The basic criteria for determining the type of biopsy that the radiologist will perform and with which imaging method the intervention will be controlled determines whether the change is palpable or not, as well as under which method the lesion in the breast is more clearly displayed. Of course, the conditions in which we work, i.e. the equipment at our disposal, are decisive in all of this, so that in some centers in Serbia, stereotaxic biopsies are not performed because the health institutions do not have the appropriate equipment.
The goal of imaging-guided biopsies is to safely provide an adequate amount of tissue required for pathohistological analysis to establish a precise diagnosis. Imaging-guided biopsies make it possible to establish a pathohistological diagnosis, which avoids the need for an “open” surgical biopsy in a high percentage, which saves money within the health system, and patients avoid unnecessary hospitalization and all the potential complications that surgical intervention entails. The experience of the Center for Imaging Diagnostics of the Institute of Oncology of Vojvodina, where these types of biopsies are performed daily, is that depending on the histopathological diagnosis, we apply excision of the change, in some cases we follow the changes intensively radiologically, or some patients return to the routine screening program. In some centers, thick needle biopsies are necessarily preceded by FNAB. If FNAB does not enable a diagnosis, or if the FNAB findings do not correlate with the clinical and radiological findings, then a biopsy with a thick needle must be performed. Of course, if microcalcifications are visualized on the patient’s mammogram, without an underlying mass, then a thick needle biopsy under mammography control (VAB) must be performed, as a standard in all centers that have this equipment.
After the biopsy, the radiologist should have an insight into the histopathological findings, in order to make a decision on further treatment in relation to the biopsied lesion. If it is proven that the change is histologically malignant, adequate oncological treatment follows, but if the radiological presentation of the change is “suspicious” BI RADS 4, and the pathohistological findings do not show any atypia or clearly indicate a malignant change, then the radiologist who performed the biopsy, brings the decision whether to monitor the change intensively radiologically or to biopsy it again. If the radiological finding is BI RADS 5 – a highly suspicious lesion, and the obtained histopathological finding after the biopsy does not confirm malignancy, then the radiologist indicates an examination with a magnet (MR mammography), repeats the biopsy or refers the patient to a consultative examination.
For the sake of more reliable findings and a better outcome for the patient, teamwork is always necessary, it is necessary for the radiologist and the pathologist to cooperate and exchange opinions on a daily basis. If there is a discrepancy between the radiological and pathological, as well as the clinical findings, there are two ways to arrive at an adequate diagnosis: either to repeat the biopsy in an identical manner, as the initial one, or biopsy with the use of a needle of a larger diameter (thicker needle). It is usual that after a core biopsy, VAB is performed in the next intervention, or (which depends primarily on the pathologist’s findings) the change is surgically excised, in order to evaluate it as a whole. There are also cases when after a biopsy with a thick needle, bearing in mind the benign histological findings, we opt for radiological monitoring. In such cases, the patient is followed by the first radiological control in 6 months. Such an approach is applied if it is a change in the breast that has grown relatively quickly, and has a benign radiological, ultrasound aspect, with a histopathological finding that it is a fibroadenoma. In that case, we consider the change to be definitely benign, but its faster growth indicates the need for ultrasound control in 6 months.
There is no point in radiologically controlling solid lesions and zones of microcalcifications in a time interval shorter than 6 months. In addition to radiologists and pathologists who decide on these changes, it is necessary to form a multidisciplinary team in the institution, which will consider each case individually and make the best decision on the further treatment of patients, in order to arrive at the right diagnosis and adequately treat the patient. A multidisciplinary team for breast diseases should consist of a surgeon, a radiologist, a pathologist, an internist-oncologist and a radiation oncologist.
Literature
1. Wallis M, Tarvidon A, Helbich T, Schreer I. Guidelines from the European Society of Breast Imaging Eur Radiol (2007) 17: 581-588.